With the US FDA estimating that nine per cent of medical device problems are directly related to use error and the actual rate of use-related errors probably much higher, Dr Anish Desai, director, Intellimed Healthcare Solutions says surgical simulation, tele-mentoring and skills training are opportunities to teach and practice advanced skills outside of the operating room as well as train surgical staff to achieve optimal patient outcomes and ensure safe usage of newer medical devices and procedures like minimally invasive surgery and robotic surgery
The adoption of technology in medicine has simplified disease management and delivered superior patient outcomes, thus giving more importance to skill development. With the complexity of newer medical devices, new technology brings out more capability and complexity that needs to be studied. Minimally invasive surgery and robotic surgery has changed the landscape of surgical interventions by making surgery more precise and less painful for the patient. An optical device/camera is needed for projection on a screen, for the surgeon to visualise the surgical field and perform the procedure. The clinical outcomes of newer procedures are both technology and skill dependant.
Talking about skills, good hand–eye coordination is critical while using slender and long instruments inserted via small incisions or natural openings. In case of a coordination problem, both, the degree of freedom and haptic feedback, are hampered, thereby affecting the outcomes of the surgery. Therefore, newer technologies need healthcare professionals to not only be competent, but also continuously upgrading their knowledge, skills and expertise. The surgical robot is probably one of the most important examples of this where surgeons have to upgrade from minimally invasive procedures.
Safety of devices and training
A use error refers to a condition in which the desired outcome after using the device is different, despite it not being dysfunctional. The error may have risen due to using a poorly designed device or incorrect usage.
As per the US FDA, nine per cent of the medical device problems are directly related to use error and the actual rate of use-related errors is probably much higher. Errors are often a result of poor equipment design, ambiguous, ill-written and disregarded warning labels, or equipment manuals. Practical use by health-care professionals or patients needs to be considered while designing medical devices. This ensures safety and can significantly reduce the errors. Hence, the most important aspect for use of medical devices/equipment is training and skill development at the operator/user level.
Training and skill development in the medtech industry
Surgical training is undergoing rapid transformation. Centuries old paradigms are challenged by legal and ethical concerns for patient safety, the cost of surgery, hospital stay and complications. Surgical simulation, tele-mentoring and skills training are opportunities to teach and practice advanced skills outside of the operating room (OR). In countries such as India, where health care has huge gaps and barriers of awareness, tools such as adoption, accessibility and affordability and tele-mentoring can be an important. Surgical tele-mentoring, a subset of telemedicine, has shown promise in recent years.
Guidelines and clinical governance protocols, accepted by the medical fraternity, are critical for training. Institutional protocols, competency of the OR and surgical team, and the types of patients treated in the hospital are also important. Another factor is the individual themselves, e.g. the surgeon`s attitude, ability for acquiring new skills and past experience.
This all makes continuous skill development, capability building and training of the relevant staff important. Training of the surgeon is most important:sSeveral learning methodologies, the use of box-trainers and practising in animal laboratories for training in laparoscopic surgery techniques facilitate the process of learning and skill development. Surgical tele-mentoring has a promising role in bridging gaps of knowledge, geographical location, accessibility and quality thus enabling mentorship in advanced procedures and newer technologies. Surgical tele-mentoring can help accelerate the learning curve.
Learning curve
A learning curve can be defined as the time taken and/ or number of procedures an average operator needs to be able to perform a procedure independently with an acceptable outcome. The learning curve depends on the complexity of the procedure and frequency of procedures performed in a time period (Figure 1). Data suggests that complication rates are inversely related to the number of the surgical cases performed. This means, the more surgeries performed, the lesser is the rate of complication.
Figure 1: Learning Curve related to design 2
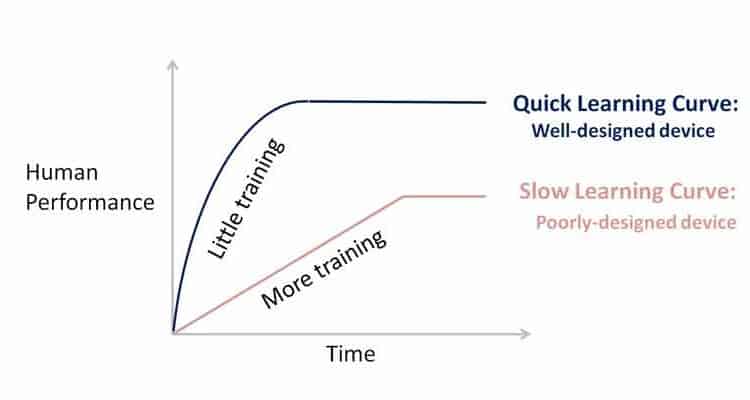
Quick Learning Curve ensures little training with a well-designed device considering human factors. Slow Learning Curve due to a poorly-designed device results in poor performance even after extensive training.
Robotic surgery has gained immense popularity in surgical fraternity. Adoption of robotic surgery requires dedicated training to achieve mastery. In a study, it was observed that the learning curve for intracorporeal knot tying in robotic surgery showed baseline laparoscopic knot completion in 140 seconds (range 47–432), whereas robotic knot tying took 390 seconds. Initial robotic training, decreased knot tying time by 65 per cent to 139 seconds. Repeated training, completion times and composite scores were improved and errors were reduced. Efficient and effective training and skill development methods have promise to address patient safety, risk management concerns, OR management, and work hours requirements.
Surgical simulators
Simulation training is as real as using actual instruments and video equipment to handle simulated “tissue” in an endo-trainer. More advanced, virtual reality simulators are now available for wider use. Systems in the past have demonstrated their effectiveness and their ability to discriminate. Newer systems enable the development of comprehensive curriculum and full procedural simulations.
Training and evaluation devices for laparoscopic surgery available are:
- Box trainers – This type of surgical simulator uses real surgical instruments and equipment including video monitors, cameras, and laparoscopes
- Animal models – These simulators involve the use of a live, anesthetised animal. This provides a realistic, non-patient environment for training.
- Virtual reality simulators – Virtual reality (VR) surgical simulators are the latest and most promising development in the area of surgical simulation.
- Full procedural simulators – Full procedural simulators go beyond the basic laparoscopic training of their predecessors and are designed to recreate the specific anatomy allowing the practicing of all skills necessary to perform a particular operation
Table 1: Surgical model for training
| Simulator model | Description | Technical aspects |
| Low fidelity | Knot trying boards | Low cost, the student can use it at home |
| High fidelity model | Human replicas
(body or specific region) |
Expensive, commercially available, maintenance cost |
| Animal model | Live animals | Expensive, ethical issues |
| Computer simulator | Interactive programs, virtual | High-cost, purchase maintenance. |
Simulation training
Development of standardised training agenda and curriculum is important especially for advanced minimal invasive surgery. Innovative approaches from experiences of the aviation industry can provide the impetus for the next generation of surgical training, ensuring the quality of the product. As the technology develops, the way we practice will continue to evolve, to the benefit of physicians and patients. Expert surgeons trained in advanced and complex procedures need to develop methods of training and evaluation that truly establish procedural based competency. It was observed that simulators improved the operating room performance of surgical residents.
The main aim of simulator training is to help trainees acquire the skills needed to perform complex minimally invasive surgical procedures prior to practicing them on living patients and accelerate the learning curve. Objectives for training are:
- Increase of knowledge spectrum;
- Learning curve;
- Time restriction;
- Student-centered learning;
- New educational techniques (simulators)
Table 2: Basic surgical abilities and number of repetitions to achieve competence
| Ability | Number of repetitions |
| Apparatus, instruments, hand hygiene, surgical hand washing, garment and gloves placement, surgical site preparation, antisepsis | 3 – 5 |
| Nasogastric tubes | 3 – 5 |
| Vesical catheter | 3 – 5 |
| Peripheral venous and arterial access | 3 – 5 |
| Central venous access | More than 10 |
| Airway access | 3 – 5 |
| Knots
Suture |
Knots 60 – 80
Suture 5 – 10 |
| Drains and wound care | 5 – 10 |
| Local anaesthesia / wound debridement | 5 – 10 |
To summarise, surgical skills training is undergoing a paradigm shift. Advances in technology has led to availability of newer devices and equipment. Appropriate training and skills development is essential to achieve optimal patient outcomes and ensure safe usage of these devices by HCPs.
References:
- Roberts KE, Bell RL, Duffy AJ. Evolution of surgical skills training. World journal of gastroenterology: WJG. 2006 May 28;12(20):3219.
- World Health Organisation. Increasing complexity of medical technology and consequences for training and outcome of care: background paper 4, August 2010. World Health Organisation; 2010.
- Advertisement -


