The service has been pared back to emergency-only, with patients screened by phone, only most acute cases seen on average 12 patients a day
Deep inside a locked-down Dunedin building, a dedicated team of Otago University dentists is operating in high-risk conditions to provide emergency dental care.
This is dangerous work and every member of the close-knit group is there voluntarily.
“We’re wired to help, it’s in our DNA, it’s what we’ve done for our whole careers,” says Dr Don Schwass, Faculty of Dentistry, Clinical Director.
The Faculty’s new clinical services building is usually buzzing with activity, undertaking more than 60,000 patient treatments each year while training dentistry students.
But under the COVID-19 restrictions, only two to four of its 281 dental chairs are in use and the dentists are working in two-hour rotations clad in specialised protective equipment.
The service has been pared back to emergency-only, with patients screened by phone and only the most acute cases seen – on average 12 patients a day.
Increasingly some of the cases are coming outside the clinic’s usual patient list, as Otago dentists find they can’t manage the risks involved with the virus or don’t have the correct protective equipment.
Where possible, patients are treated medically by prescription over the phone and there is a tight definition of what qualifies as a dental emergency. This includes severe infections with a swollen face, severe pain not managed by pain relief, trauma and bleeding that won’t resolve.
When an emergency patient is seen in the clinic, the team has severely limited treatment options. For example, drills can’t be used because the high-speed rotation whips up the air which could then spread the virus.
It’s a sobering thought that in the UK already an ENT specialist has died after being infected while treating patients.
“Working in the mouth is one of the more high-risk things that you can do with the virus in the community. So it’s basically hand instruments, dressings and extractions.”
In addition to the infection risk, the team is under pressure to make decisions with the limited tools and treatment choices available.
“It’s really compromising what we can offer and patients are having to understand that compromise. So whereas you might save a tooth with a root canal we can’t do that. So the only option, if antibiotics and pain relief doesn’t work, is to remove the tooth.”
Overall a team of 40 is involved in providing the service, ranging from administrative staff all the way up to dedicated maxillofacial consultant team.
To manage stress and workloads, the volunteers are working in two hours shifts with a set number of patients before a rest period.
They are only too aware that the Southern region has the highest number of COVID-19 cases in New Zealand and that it’s probable the situation will get worse before it improves.
Dr Schwass says the team is busy but managing the workload and has the capacity to grow if needed.
With that in mind, a mobile dental clinic is being set up as a precaution outside the clinical services building. This will be brought into use if the virus spread reaches the point where it has to be assumed that all patients potentially have the virus.
Due to the design of the new clinic facility and its ventilation system, it is too risky for patients to make the trip into the clinical services building.
Only patients considered low risk are seen in the clinical services building, whereas the mobile unit offers a full containment environment for managing high-risk patients.
In the meantime, it’s a matter of taking each day as it comes, a small team doing vital work in one corner of a large empty building.
“Everyone’s got each other’s back and one of the guiding principles is that everyone is keeping an eye on everyone else’s cross infection control observance and making sure that everyone stays safe. Because lives are on the line, literally.”
- Advertisement -


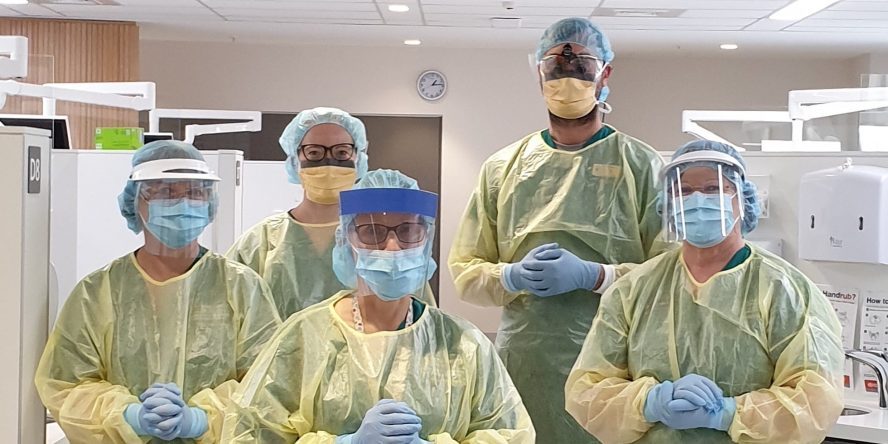
Due to COVID most of the Dental clinics are shut down and kudos to this team who are working selflessly, solving the dental problems of the patients. It was an amazing read indeed and I will definitely share the same with my family.